Is junctional rhythm normal
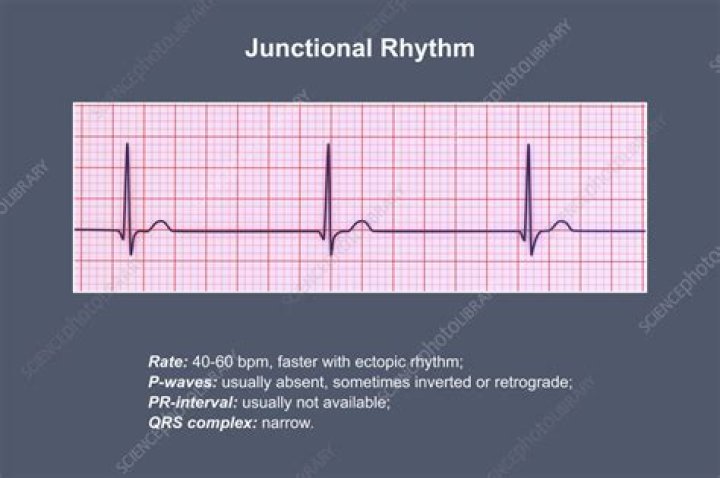
A junctional rhythm is normally slow — less than 60 beats per minute. When faster, it is referred to as an accelerated junctional rhythm.
What is the significance of junctional rhythm?
A predominant junctional rhythm may be associated with structural heart disease, sick sinus syndrome, or both, during which the junctional escape rhythm supersedes the sinus rate and provides a safety mechanism.
Is a junctional rhythm an emergency?
A Junctional rhythm can happen either due to the sinus node slowing down or the AV node speeding up. It is generally a benign arrhythmia and in the absence of structural heart disease and symptoms, generally no treatment is required.
What are the symptoms of junctional rhythm?
Junctional rhythm can cause symptoms due to bradycardia and/or loss of AV synchrony. These symptoms (which can be vague and easily missed) include lightheadedness, palpitations, effort intolerance, chest heaviness, neck tightness or pounding, shortness of breath, and weakness.Can anxiety cause junctional rhythm?
An issue with your heart’s electrical wiring system can lead to junctional tachycardia. You may be born with it, or it might happen later. Drug use or anxiety could trigger the condition.
Can atrial flutter cause stroke?
Atrial flutter is a type of abnormal heart rhythm, or arrhythmia. It occurs when a short circuit in the heart causes the upper chambers (atria) to pump very rapidly. Atrial flutter is important not only because of its symptoms but because it can cause a stroke that may result in permanent disability or death.
Is a junctional rhythm a heart block?
Other than the above-listed causes of severe SA node disease, which can result in junctional rhythm, a high-grade second-degree heart block and a third-degree heart block can also result in a junctional rhythm.
What are the lethal dysrhythmias?
Ventricular tachycardia (VT) and ventricular fibrillation (VF) are lethal cardiac arrhythmias, claiming a quarter million lives per year from sudden cardiac death (SCD).Can junctional rhythm have PAC?
Like the premature atrial contraction (PAC), the premature junctional beat is characterized by a premature, abnormal P wave and a premature QRS complex that’s identical or similar to the QRS complex of the normally conducted beats, and is followed by a pause that is usually noncompensatory.
What happens if AV node is blocked?Symptoms. The symptoms of AV block are similar to sick sinus syndrome (SSS), and are a direct product of the resultant slow heart rates. These include palpitations, skipped-beats, dizziness, lightheadedness, syncope (loss of consciousness), fatigue and weakness, confusion, and even angina (chest pain).
Article first time published onIs Sinus Arrhythmia serious?
Keep in mind that for the majority of people, a sinus arrhythmia is neither dangerous nor problematic. Even if your doctor suspects you have this irregular heartbeat, he may not order the test to check for it. That’s because an EKG can be costly, and a sinus arrhythmia is considered a benign condition.
What is the most lethal heart rhythm?
Fatal or potentially fatal arrhythmias The most dangerous arrhythmia is ventricular fibrillation, in which your ventricles quiver rather than beat steadily in time with your atria. Your ventricles will stop pumping blood to the rest of your body, including your heart muscle.
How fast is junctional tachycardia?
In general, the AV junction’s intrinsic rate is 40-60 bpm so an accelerated junctional rhythm is from 60-100bpm and then becomes junctional tachycardia at a rate of >100 bpm.
Is wandering atrial pacemaker regular?
RateVariable depending on the site of the pacemaker; usually 45-100/ bpm.QRSNormalConductionP-R interval varies depending on the site of the pacemaker
What are the symptoms of third degree heart block?
- light-headedness.
- dizziness.
- fainting.
- fatigue.
- chest pain.
- slow heart beat (bradycardia)
What causes AFib RVR?
Rapid ventricular rate or response (RVR) AFib is caused by abnormal electrical impulses in the atria, which are the upper chambers of the heart. These chambers fibrillate, or quiver, rapidly. The result is a rapid and irregular pumping of blood through the heart.
When should you worry about an irregular heartbeat?
“If you have symptoms of lightheadedness, chest pain, or shortness of breath along with an irregular heart rhythm, then seek help immediately,” says Mitiku. “You may have to be evaluated for the more dangerous arrhythmias or sudden cardiac arrest.”
Are heart palpitations and arrhythmia the same thing?
A heart that beats irregularly, too fast or too slow is experiencing an arrhythmia. A palpitation is a short-lived feeling like a feeling of a heart racing or of a short-lived arrhythmia.
When should I be worried about heart palpitations?
If your palpitations are accompanied by dizziness, fainting, shortness of breath, or chest pain, you should seek medical attention. “Palpitations can be caused by a wide range of abnormal heart rhythms.
How do you treat junctional tachycardia?
Congenital junctional ectopic tachycardia (JET) is usually initially treated with antiarrhythmic therapy, with the choice of medication guided by the degree of coexisting ventricular dysfunction. Congenital JET has been successfully controlled with amiodarone, propafenone, or cautious combinations of both medications.
Is a sinus rhythm good?
It means the electrical pulse from your sinus node is being properly transmitted throughout the heart muscle. In adults, normal sinus rhythm usually accompanies a heart rate of 60 to 100 bpm. However, it’s possible for sinus rhythm to be faster or slower than this and still be considered normal.
How long can you live with atrial flutter?
Most patients with atrial flutter lead an entirely normal life with modern drugs and treatments.
Is atrial flutter life threatening?
Although atrial flutter is usually not life-threatening at first, it does limit how well your heart pumps blood. This can cause a clot to form in your heart. If the clot breaks loose, it could lead to a stroke.
Can caffeine cause fluttering?
Research suggests that caffeine isn’t a cause of abnormal heart rhythms or atrial fibrillation, and drinking four to five cups of tea or coffee a day shouldn’t increase your risk of developing coronary heart disease either.
What do PJCs look like?
PJCs have the following features: Narrow QRS complex, either (1) without a preceding P wave or (2) with a retrograde P wave which may appear before, during, or after the QRS complex. If before, there is a short PR interval of < 120 ms and the “retrograde” P waves are usually inverted in leads II, III and aVF.
What causes 3rd degree heart block?
Third-degree heart block may be caused by: Damage to the heart from surgery. Damage to the heart muscle from a heart attack. Other types of heart disease that result in heart muscle damage.
What is a PJC heart?
A premature junctional complex (PJC) is an abnormality seen in the presence of an underlying sinus rhythm. It is an aberrant impulse that originates in the atrioventricular junction (junctional tissue) and occurs early or prematurely before the next expected P wave.
Is Pea a lethal rhythm?
The overall mortality rate is high in patients in whom PEA is the initial rhythm during cardiac arrest. In a study by Nadkarni et al, only 11.2% of patients who had PEA as their first documented rhythm survived to hospital discharge.
Can you do CPR on asystole?
Asystole is treated by cardiopulmonary resuscitation (CPR) combined with an intravenous vasopressor such as epinephrine (a.k.a. adrenaline). Sometimes an underlying reversible cause can be detected and treated (the so-called “Hs and Ts”, an example of which is hypokalaemia).
Can a heart vibrate?
Atrial Fibrillation is a quivering or irregular heartbeat (arrhythmia) that can lead to blood clots, stroke, heart failure, and other heart-related complications.
Is AV node ablation safe?
AV Node ablation is also a very common and very low risk procedure. Although most people undergoing AV node ablation do not experience any complications, you should be aware of the following risks: Local bleeding, blood clot or haematoma (blood collection) – this may occur at the catheter insertion site.



