What causes tubular atrophy
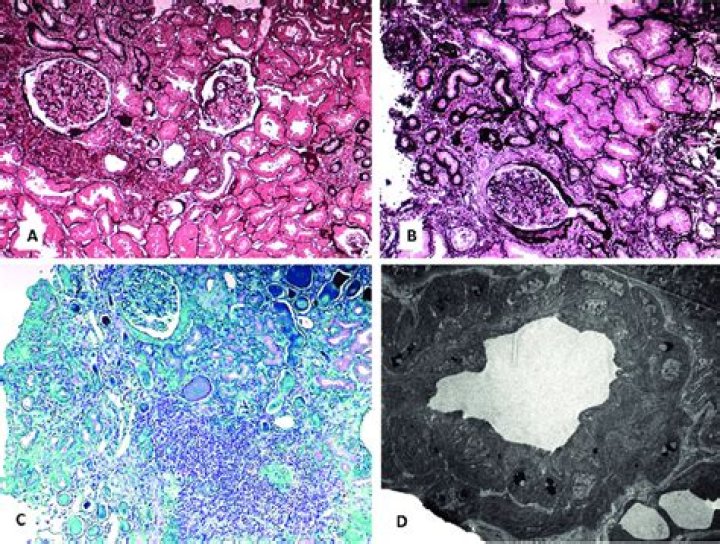
Tubular atrophy is a general term that describes several patterns of chronic tubular injury with thickened tubular basement membranes, and clinically manifests as chronic kidney disease with decreased glomerular filtration rate.
What is tubular atrophy in kidney?
Tubular atrophy is a general term that describes several patterns of chronic tubular injury with thickened tubular basement membranes, and clinically manifests as chronic kidney disease with decreased glomerular filtration rate.
What causes interstitial fibrosis kidney?
Renal fibrosis, particularly associated with glomerulosclerosis and renal interstitial fibrosis (5,10,27,28) that is characterised by tubular atrophy, tubular dilatation, increased fibrogenesis (29) and deposition of collagen and ECM (15), can progress in humans as a consequence of chronic infection, obstruction of the …
What is mild interstitial fibrosis and tubular atrophy?
Interstitial fibrosis and tubular atrophy (IF/TA), previously included within the term chronic allograft nephropathy, is a common histological abnormality of kidney transplants in which an expanded interstitial space replaces normal cortical structures.What causes chronic glomerulonephritis?
Glomerulonephritis may develop a week or two after recovery from a strep throat infection or, rarely, a skin infection (impetigo). To fight the infection, your body produces extra antibodies that can eventually settle in the glomeruli, causing inflammation.
What is acute tubular necrosis?
Acute tubular necrosis (ATN) is a kidney disorder involving damage to the tubule cells of the kidneys, which can lead to acute kidney failure. The tubules are tiny ducts in the kidneys that help filter the blood when it passes through the kidneys.
Is renal scarring permanent?
Renal scarring can be a permanent consequence of urinary tract infection (UTI), and is associated with long-term conditions such as decreased renal function and hypertension.
What does interstitial lung disease?
Interstitial lung disease (ILD) is an umbrella term used for a large group of diseases that cause scarring (fibrosis) of the lungs. The scarring causes stiffness in the lungs which makes it difficult to breathe and get oxygen to the bloodstream. Lung damage from ILDs is often irreversible and gets worse over time.What are symptoms of fibrosis?
- Shortness of breath (dyspnea)
- A dry cough.
- Fatigue.
- Unexplained weight loss.
- Aching muscles and joints.
- Widening and rounding of the tips of the fingers or toes (clubbing)
- Fatigue.
- High blood pressure.
- Swelling of the face, hands, feet, and belly.
- Blood and protein in the urine (hematuria and proteinuria)
- Decreased urine output.
How common is renal fibrosis?
Surprisingly, 13.9% of patients with normal renal function had 25-49% fibrosis and 5% had more than 50% fibrosis on biopsy, and 5 years after undergoing biopsy 21% of patients with >50% fibrosis still remained dialysis free.
How is renal fibrosis treated?
There are currently no drugs for CKD and fibrosis in clinical use that would specifically target the kidney. Despite a number of potential anti-fibrotic treatment targets identified in preclinical studies, translation to clinical trials has remained remarkably poor.
Why is kidney fibrosis bad?
Renal fibrosis is a direct consequence of the kidney’s limited capacity to regenerate after injury. Renal scarring results in a progressive loss of renal function, ultimately leading to end-stage renal failure and a requirement for dialysis or kidney transplantation.
What drugs can cause glomerulonephritis?
Drug class/drug(s)Pathophysiologic mechanism of renal injuryAllopurinol (Zyloprim)Acute interstitial nephritisGold therapyGlomerulonephritisHaloperidol (Haldol)RhabdomyolysisPamidronate (Aredia)Glomerulonephritis
Can autoimmune disease cause kidney stones?
In sarcoidosis, immune system cells form lumps called granulomas. The lumps collect in various organs, sometimes including the kidneys. Sarcoidosis can harm the kidneys. It also may lead to kidney stones because of extra calcium in the urine.
Is glomerulonephritis an autoimmune disorder?
Glomerulonephritis is often an autoimmune condition; in other words, it is caused by the body’s immune system attacking its own tissues.
How do you treat kidney scarring?
- Immune system medicines. …
- Dialysis. …
- Kidney transplant. …
- Blood pressure lowering medicines.
- Diet changes.
How does kidney scarring happen?
Kidney scarring, or ‘fibrosis’ is the primary cause of kidney disease and is triggered by factors including diabetes, autoimmune disease and high blood pressure, regular use of certain medications and prolonged infections.
Do scarred kidneys hurt?
Scarring usually does not cause pain. It can on rare occasions lead to impaired function of an organ if the scarring is extensive. When this occurs in the kidney, it is usually the result of an infection within the kidney tissue.
What is the most common cause of acute tubular necrosis?
The most frequent causes of acute tubular necrosis are a stroke or a heart attack, conditions that reduce oxygen to the kidneys. Chemicals can also damage the tubules.
Can dehydration cause acute tubular necrosis?
Events such as diarrhea, vomiting, sepsis, dehydration, or bleeding that leads to tissue hypoxia can indicate a risk of acute tubular necrosis.
What are the three phases of acute tubular necrosis?
- Onset or initiating phase. Lasting hours or days, this is the time from onset of the precipitating event (for example, toxin exposure) until tubular injury occurs.
- Maintenance phase. …
- Recovery phase.
What are the first signs of pulmonary fibrosis?
The most common symptoms of pulmonary fibrosis are dry, persistent cough and shortness of breath. Symptoms may be mild or even absent early in the disease process. As the lungs develop more scar tissue, symptoms worsen.
How do you test for fibrosis?
- Chest X-ray. A chest X-ray shows images of your chest. …
- Computerized tomography (CT) scan. CT scanners use a computer to combine X-ray images taken from many different angles to produce cross-sectional images of internal structures in the body. …
- Echocardiogram.
Can Covid cause lung fibrosis?
The persistent respiratory complications may cause substantial population morbidity, long-term disability, and even death due to the lung fibrosis progression. The incidence of COVID-induced pulmonary fibrosis caused by COVID can be estimated based on a 15-year observational study of lung pathology after SARS.
What is the life expectancy of someone with interstitial lung disease?
The average survival for people with this type is currently 3 to 5 years . It can be longer with certain medications and depending on its course. People with other types of interstitial lung disease, like sarcoidosis, can live much longer.
What is the best test to confirm interstitial lung disease?
Computerized tomography (CT) scan. This imaging test is key to, and sometimes the first step in, the diagnosis of interstitial lung disease. CT scanners use a computer to combine X-ray images taken from many different angles to produce cross-sectional images of internal structures.
Can interstitial lung disease come on suddenly?
Interstitial lung disease can be acute (coming on suddenly) or chronic (occurring over time).
What autoimmune diseases cause kidney problems?
Lupus nephritis is a frequent complication in people who have systemic lupus erythematosus — more commonly known as lupus. Lupus is an autoimmune disease. It causes your immune system to produce proteins called autoantibodies that attack your own tissues and organs, including the kidneys.
Which is the main complication of glomerulonephritis?
Glomerulonephritis is a type of kidney disease. It involves damage to the glomeruli (tiny filters) inside your kidneys. If you have glomerulonephritis, your kidneys can have trouble removing waste and fluid from your body. If the condition becomes severe, it can lead to kidney failure.
What is Bright's disease?
Acute nephritis occurs when your kidneys suddenly become inflamed. Acute nephritis has several causes, and it can ultimately lead to kidney failure if it’s left untreated. This condition used to be known as Bright’s disease.



