What is homocysteine resist
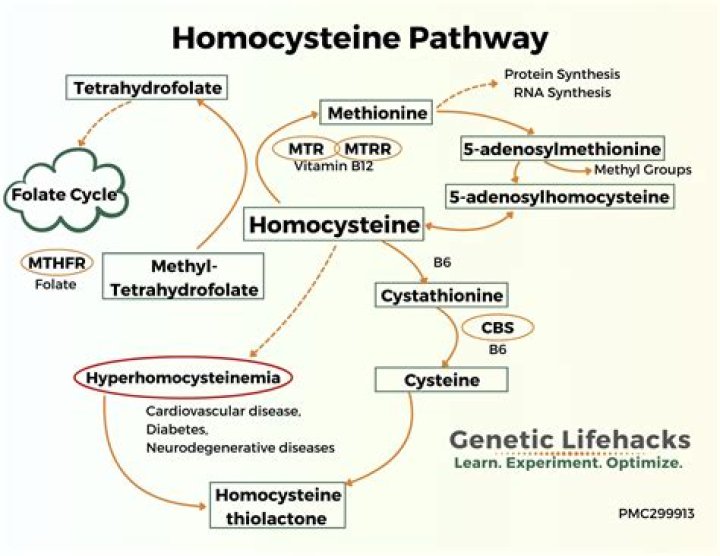
Homocysteine is an amino acid. Vitamins B12, B6 and folate break down homocysteine to create other chemicals your body needs. High homocysteine levels may mean you have a vitamin deficiency. Without treatment, elevated homocysteine increases your risks for dementia, heart disease and stroke.
What is homocysteine and what is its function?
Homocysteine is an amino acid. Vitamins B12, B6 and folate break down homocysteine to create other chemicals your body needs. High homocysteine levels may mean you have a vitamin deficiency. Without treatment, elevated homocysteine increases your risks for dementia, heart disease and stroke.
What is homocysteine supreme for?
Homocysteine Supreme maintains a healthy homocysteine pathway, allowing for the normal production of its necessary and important end products. These include the sulfur-containing amino acids taurine and cysteine, and the neurotransmitters norepinephrine and dopamine.
What are the side effects of homocysteine?
Nausea, stomach upset, diarrhea, drowsiness, flushing, and numbness/tingling may occur. If any of these effects persist or worsen, notify your doctor or pharmacist promptly.What are the symptoms of high homocysteine?
- pale skin.
- weakness.
- fatigue.
- tingling sensations (like pins and needles) in the hands, arms, legs, or feet.
- dizziness.
- mouth sores.
- mood changes.
Does homocysteine cause blood clots?
Elevated levels of homocysteine show an increased risk for (1) hardening of the arteries (atherosclerosis), which could eventually result in a heart attack and/or stroke, and (2) blood clots in the veins, referred to as venous thrombosis.
Why is homocysteine bad?
Raised levels of homocysteine are also linked to Alzheimer’s, dementia, declining memory, poor concentration and judgment and lowered mood. Women with high homocysteine levels find it harder to conceive and are at risk from repeated early miscarriage.
Does homocysteine cause inflammation?
Background: An elevated level of homocysteine (Hcy) has been shown to be a cardiovascular risk factor in the majority of research studies. Recently, it was found to be associated with new risk factors such as inflammatory markers.Does exercise lower homocysteine?
Although exercise increases homocysteine short-term, in the long term, it is associated with lower homocysteine levels. A systematic review of 34 studies found that regular exercise may be able to decrease homocysteine levels [91].
When should I take homocysteine supreme?- Bottle Volume. 120 Capsules.
- Suggested Use: As a dietary supplement, take two capsules daily, with meals, or as directed by your healthcare practitioner.
- Precautions. Consult your healthcare practitioner before use, especially if you are pregnant or nursing.
What diagnosis covers homocysteine?
Homocysteine levels will be covered by Medicare to confirm Vitamin B12 or folate deficiency.
Which foods reduce homocysteine?
Studies show foods containing folic acid may lower homocysteine. Try beans, leafy green vegetables, citrus fruits, beets, and wheat germ. A controlled trial showed that eating a diet high in fruits and vegetables containing folic acid, beta-carotene and vitamin C effectively lowered homocysteine levels.
How can I lower my homocysteine levels naturally?
- Many breakfast cereals.
- Fortified grain products.
- Lentils.
- Asparagus.
- Most beans.
What are symptoms of low homocysteine?
- weakness.
- dizziness.
- sores on mouth or tongue.
- tingling in the feet, legs, hands, or arms.
- fatigue.
- pale skin.
Does exercise increase homocysteine?
Current evidence demonstrates that acute exercise increases homocysteine levels in the blood independent of exercise duration and intensity. Resistance, but not aerobic training decreases plasma homocysteine levels.
Which vitamins reduce homocysteine?
The good news: Homocysteine can be lowered easily and inexpensively with a trio of B vitamins — B6, B12, and folic acid.
Can stress raise homocysteine levels?
The study of 34 middle-aged women found that brief periods of stress increased blood levels of the amino acid homocysteine. Research over the past 20 years has found that an even moderately elevated level of homocysteine is a risk factor for heart disease in both men and women.
What blood test shows homocysteine?
The homocysteine blood test helps diagnose B6 and B12 Deficiency, as well as, a Folate Deficiency. It is also used to identify patients who may be at risk for heart disease and/or strokes. Patients are advised to fast for 8-10 hours prior to the homocysteine blood test. Results are available in one to two days.
Can high homocysteine levels cause high blood pressure?
Homocysteine may elevate blood pressure by damaging vascular endothelial integrity (6–9), increasing arterial stiffness (7,10,11), and reducing vasodilatory capacity (8,12).
Does walking reduce homocysteine?
Duncan et al50 found that 6 months of exercise increased homocysteine levels in sedentary adults, whereas Randeva et al51 showed that 6 months of sustained brisk walking for 20 to 60 minutes 3 days a week significantly decreased homocysteine levels and increased CVF in young overweight and obese women with polycystic …
Does caffeine raise homocysteine levels?
Conclusions: Caffeine is partly responsible for the homocysteine-raising effect of coffee. Coffee, but not caffeine, affects homocysteine metabolism within hours after intake, although the effect is still substantial after an overnight fast.
What is ideal homocysteine level?
Most laboratories report normal homocysteine levels in the blood between 4 and 15 micromoles/liter (µmol/L). Any measurement above 15 is considered high. Any measurement below 12 is considered low. Optimal homocysteine levels are below 10 to 12.
Is homocysteine an inflammatory marker?
Since inflammation promotes cell proliferation at the expense of excess vitamins leading to hyperhomocysteinemia, therefore, homocysteine can be used as a marker of inflammation to indicate the presence of inflammation.
What converts homocysteine to methionine?
Methionine synthase is a cobalamin-dependent enzyme that catalyzes the conversion of homocysteine to methionine.
Is homocysteine an acute phase reactant?
Conclusion: Although homocysteine plasma values obtained during the sixth and twelfth hours of acute myocardial infarction provide reliable results as a risk markers, timing of blood sampling during the myocardial infarction does not have significant role since plasma values of homocysteine did not affect acute phase …
Does vitamin B12 lower homocysteine?
Supplementation with vitamins B9, B12, and B6 appears to decrease the homocysteine levels and potentially contributes to stroke prevention although direct evidence is lacking [12, 13]. Vitamin B12 deficiency can be detected in 10–40% of the general population and may contribute to stroke and cognitive decline [14, 15].
How are folic acid B12 and homocysteine related?
Vitamin B12 deficiency, therefore, can lead to increased levels of serum methylmalonic acid. In the second reaction, homocysteine is converted to methionine by using vitamin B12 and folic acid as cofactors. In this reaction, a deficiency of vitamin B12 or folic acid may lead to increased homocysteine levels.
Are B12 shots covered by Aetna?
Aetna considers vitamin B-12 injections experimental and investigational for all other indications, including use for the treatment of age-related cataract, amyotrophic lateral sclerosis, autism, chronic fatigue syndrome (myalgic encephalomyelitis), delayed sleep-wake phase disorder, non-24-hour sleep-wake rhythm …
What ICD 10 code covers homocysteine?
E72. 11 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
Does Aetna cover homocysteine?
Aetna considers homocysteine testing (measurements of plasma homocysteine) medically necessary for the following indications: Assessment of borderline vitamin B12 deficiency, where the results will impact the member’s management (see CPB 0536 – Vitamin B-12 Therapy); or.
Does zinc lower homocysteine?
With zinc supplementation, homocysteine levels reduced significantly (from 13.71 ± 3.84 μmol/l to 11.79 ± 3.06 μmol/l; p < 0.05), which did not occur on placebo (from 12.59 ± 2.13 μmol/l to 13.36 ± 2.03 μmol/l).